In 1953, the American anesthesiologist Virginia Apgar published an article in which she proposed a new system for assessing the condition of a newborn. In recognition of her work, this system is called the Apgar scale.
What parameters are included on this scale?
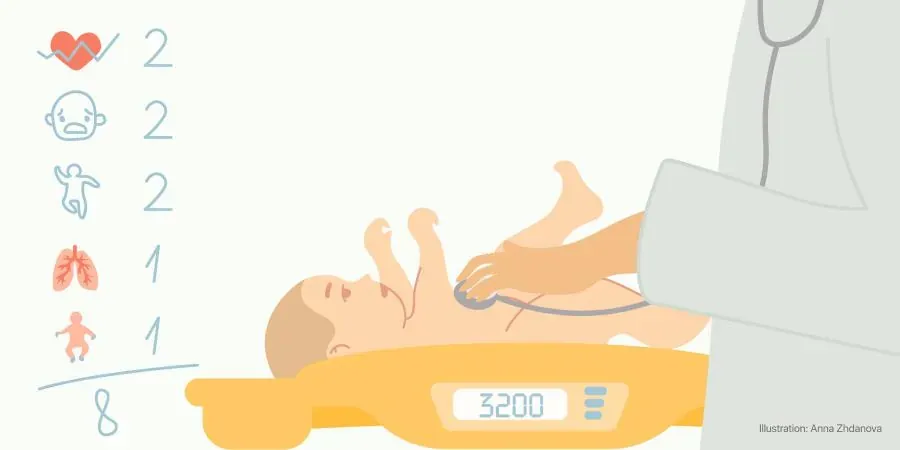
Before Apgar, the condition of newborns was evaluated very subjectively: good, good-bad, bad. Dr. Apgar suggested five parameters that can be measured quickly, without performing any complex manipulations with the newborn. And at the same time, they allow you to fairly objectively assess the condition of the baby. Each indicator is rated from 0 to 2 points, and their sum makes up the Apgar score [1].
Pulse. More than 100 beats per minute is given two points, less than 100 beats per minute is given one point, no pulse is zero. It is most reliable to measure the pulse at the umbilical cord about 5 cm from the navel.
Breathing. Immediate screaming and breathing actively is given two points. If at one minute post birth, the baby does not breath, zero points. Everything else in between is given one point.
Reflexes. When the Apgar method was first developed, fluid was pumped out of the nose and mouth of newborns with a rubber catheter. A normal reaction was considered to be coughing or sneezing (two points). Urination or defecation was not considered the "correct" response to such a stimulus, but was given one point. No reactions — zero points. Now, it is more common to run a finger along the sole of the baby (tickle the heel). Two points if the baby shouts and kicks; one point if the baby responds with some movement. Zero if there is no reaction. At the fifth minute, the child's reactions are usually more expressive than immediately after birth, and the Apgar score increases [2].
Muscle tone. If there is none, zerio points; good tone, one point; if you bend baby’s arms and legs and they resist extension, two points.
Color. If baby is completely pale and blue, zero points; if baby has blue hands or feet, but the rest of the body is pink and well-colored, one point. Two points are given if the child is completely pink. But immediately after birth, many babies are completely cyanotic, and after 3-5 minutes they gain their natural color. According to Dr. Apgar, color is the least indicative criterion. Even if the child had 2 points for everything else, baby’s color may receive zero points on color.
The first Apgar score at birth is taken 60 seconds after birth and then again five minutes later. For this reason, the results are written as two numbers separated by a fraction. For example: 8/9.
The Apgar score is related to the probability of a child's death shortly after birth: the higher the score, the lower the risk [1]. If the total is two points or less, the baby needs resuscitation. From three to seven points, baby requires medical supervision. Above seven means the baby is healthy. The second estimate five minutes after birth is considered more reliable.
Usually, lower Apgar scores are combined with already known risk factors. Often, baby with following risk factors do not reach seven points:
small babies (less than 5 lbs 8 oz);
large babies (more than 9 lbs 14 oz);
breech babies;
second child of twins;
babies born after 40 weeks of pregnancy;
babies of smoking mothers [3].
On the Apgar scale, can you predict the likelihood of future diseases?
The scale was created primarily to predict the viability of the baby for the first month of life [1]. After that, a lot depends on the quality of medical care and living conditions. The relationship between the Apgar score and the probability of neurological diseases has been studied for many years [2, 4] and researchers have found that the Apgar scale has a poor predictive value — only 12%.