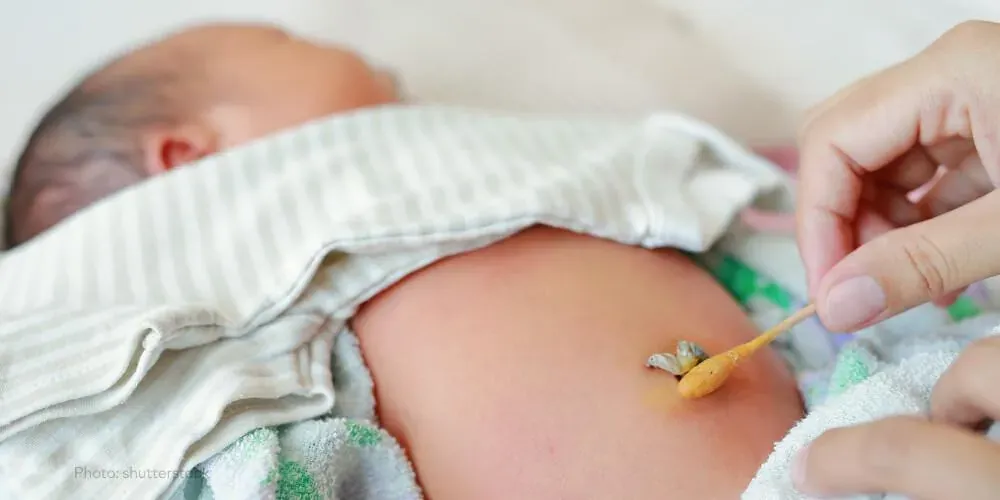
The final stage of labor is birthing the placenta. This temporary organ allowed you to communicate with baby, and now that you can communicate directly, you no longer need the placenta. Birthing the placenta is often brief, but intense.
How does this happen?
The walls of the uterus continue to contract intensely, as if trying to separate the placenta from your body. As soon as the contractions succeed, the last urge to push comes and the placenta passes through the birth canal. Now the birth is really over. But you will still feel something like contractions for a while: this is the muscles of the uterus contracting to squeeze the vessels and prevent blood loss. A little blood loss is inevitable.
To reduce blood loss, the WHO approves of medical intervention at the last stage of childbirth. For example, all over the world, it is customary to administer oxytocin to a mother immediately after the birth of a child: this hormone increases uterine contractions and, consequently, reduces bleeding [1].
Is it possible to give birth to a placenta without medical intervention?
Yes. By and large, there are two extremes in the management of the last stage of labor: expectant and active. And there are range compromises between them. So far, there is no evidence that any strategy is better than the other [2].
The wait-and-see tactic assumes a completely physiological course of labor. It is popular in Scandinavia and New Zealand, and is also practiced in many countries for home births. And in low-income regions, it is common simply for lack of choice. The main principle of wait-and-see tactics can be formulated as "do not touch with your hands".
What’s not allowed:
administration of oxytocin;
squeeze the umbilical cord until it stops pulsating;
pulling the placenta by the umbilical cord.
To stimulate the production of a woman's own oxytocin, the baby is immediately applied to the breast — the hormone is produced in response to sucking [2].
And what does an active intervention tactic look like?
With the active management of the last period of labor, everything is done exactly the opposite:
oxytocin is administered immediately after the birth of the child;
squeeze or cut the umbilical cord (that is, they artificially stop the pulsation of blood in it);
gently pull the placenta out by the umbilical cord [2].
What tactics are used more often?
Most often, obstetricians try to combine these tactics in different ways. For example, some may administer oxytocin, but not squeeze the umbilical cord or pull it out. Others may skip the oxytocin, but pinch the umbilical cord immediately and pull it to help remove the placenta. Others still may give oxytocin, squeeze the umbilical cord and thereby accelerate the birth of the placenta without any pulling. There are many options.
The latest WHO recommendations [1] are to administer oxytocin but not cut the umbilical cord immediately, but also not to wait for the pulsation to stop — just delay the squeezing of the cord for one minute. At the same time, pulling the placenta by the umbilical cord is allowed only for very experienced obstetricians.
Which is best? Cut the umbilical cord first and then wait for the birth of the placenta, or vice versa?
It depends on the chosen tactics. The umbilical cord can be cut immediately after birth, a minute after birth, after the end of the pulsation of blood in the umbilical cord, or even after the birth of the placenta. It is believed that after clamping the umbilical cord (after it has ceased to provide a connection between the mother and the child), the placenta separates somewhat faster [2].
What is the point of delaying the cutting of the umbilical cord?
Through the umbilical cord, the baby receives a portion of blood from the mother. As a result, it increases the level of hemoglobin and iron, reducing the risk of anemia both immediately after birth and at the age of six months. In general, delayed cord clamping in premature infants reduces mortality rates [3].